The concept of pre-warming composite resin has been around for many years. Woodlum, Berry, and others described the benefits of preheating composite resins prior to placement in 2008.1 Amalgam is condensable and adapts well to a geometric cavity preparation when placed, but composite resins do not behave in a similar fashion. Placing composite in a cavity preparation is a bit like pushing around mashed potatoes. As material science has worked to make composite materials more condensable by increasing the viscosity of the material (condensable or packable composites), this can present the problem of imprecise adaptation to the complex geometry of the cavity preparation. It is thought that the reported shorter clinical lifespan of composite restorations when compared to amalgam is in part due to this imprecise adaptation, which can lead to an increased susceptibility for microleakage and recurrent decay.2 Therefore, adaptation is definitely the main reason to consider composite warming. By increasing the temperature of the composite resin to 155°F (68°C), the viscosity of the material is sufficiently reduced, allowing for precise adaptation the cavity preparation without condensing. Once the heat dissipates, the composite stiffens and becomes more sculptable, allowing the clinician to more easily create esthetic tooth shapes in the uncured material without slumping. When restoring Class II cavity preparations, the use of warmed composite can greatly facilitate the adaptation of the material in the gingival floor of the proximal box and at the line angles where the gingival floor meets the facial and lingual (palatal) vertical walls.3 Incomplete fill due to hand condensing in these areas is not always clinically or radiographically evident until later in the life of the restoration, when microleakage can lead to recurrent decay and ultimate failure of the restoration. With the advent of low-shrink, bulk-fill paste composites, which can be placed in a single increment up to 4 mm in thickness, warming these materials prior to placement and filling the entire cavity preparation with marginal accuracy in one increment is now possible. Better adaptation and the elimination of layering means that the clinician can create a direct “monolithic” restoration very close to its indirect counterpart but delivered in a single patient visit.
Warming of composite positively changes the physical or mechanical properties of the material. It significantly increases the monomer conversion rate on the surface and the bottom of the restorative material, which can lead to improved surface microhardness, better flexural strength, and an increased depth of cure,4,5 all important considerations when considering the longevity of the restorative material. Preheating has also been shown to reduce microleakage and internal voids in the composite material.6-8
Anterior Tooth Anatomy and Matrix Options
Rebuilding natural appearing anterior interproximal surfaces (Class III or Class IV cavities) with direct composite presents many inherent challenges to the clinician. The emergence profiles, which are concave below the gingival crest, then convex in the gingival embrasure as the proximal surface extends incisally toward the contact area, are impossible to reproduce using traditional direct composite placement techniques and flat mylar matrix strips with wedges. Also, the limited access to the interproximal area with composite finishing burs, abrasive discs, and contouring strips also make it extremely difficult to modify and properly finish natural free flowing anatomic surfaces. Lastly, shade matching a portion of a multicolored tooth with varying opacities from cervical margin to incisal edge is very difficult using traditional direct composite armamentarium when trying to replicate natural tooth characterization.
Re-Creating Anterior Proximal Surfaces and Emergence Profile in Composite Resin
Traditional flat mylar strips or preformed celluloid crown forms have been the only matrix choices for anterior direct composite restorations since composite resin has been in use. The limitations of these matrices are obvious. Mylar strips are flat and cannot properly reconstitute concave and convex physiologic profiles to the restorative material. The result is flat surfaces and “black triangles” between anterior teeth. Celluloid crown forms are not customizable enough to be used in all situations because of the extreme amount of variability in tooth size and morphology. A unique set of matrices (Bioclear, Bioclear Matrix Systems) can be effectively used to reproduce proximal physiological contours and create esthetic diastema closures when using direct composite. This matrix is a 50-micron mylar material that is placed in intimate contact with the tooth (root) structure and held in place with the rubber dam. No interproximal wedge is used, as the compression would distort the shape of the matrix. The latex material tightly holds the matrix in contact to the tooth surface so that there will be a flawless transition from tooth to restorative material as the convex emergence profile of the composite leaves the tooth surface.
Maxillary Lateral Incisor Restoration Using Warmed Composite: A Case Report
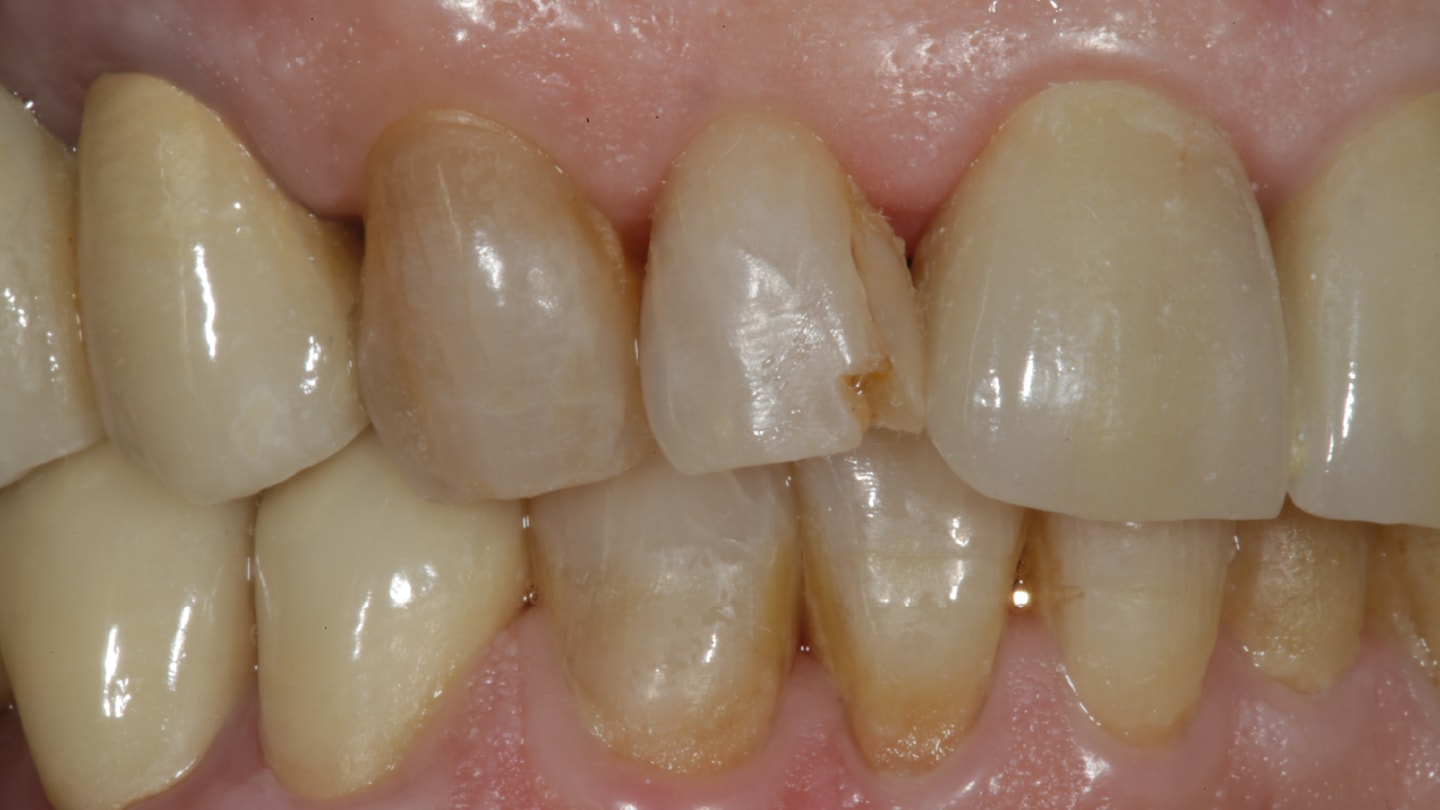
A patient presented with an existing fractured Class IV mesial restoration on tooth No. 7 (Figure 1). The operative plan is to use a single-shade composite (OMNICHROMA, Tokuyama Dental) for this case to re-create natural contours and esthetics because of the material’s ability to seamlessly blend with the natural portion of the tooth. After removal of the existing material and modification of the cavity preparation, isolation is performed using rubber dam (MiniDam, DMG America). An anatomic mylar matrix (Bioclear) is positioned below the gingival margin and stabilized with an interproximal wedge (Bioclear Diamond Wedge, Bioclear Matrix Systems) (Figure 2). The preparation is etched with 37% phosphoric acid for 15 seconds, then thoroughly rinsed and air dried, with care taken not to desiccate the surface of the dentin. A bonding resin (Bond Force, Tokuyama Dental) is copiously applied to the surface of the preparation (Figure 4), air thinned, then light cured per manufacturer’s specifications (Figure 5). Figure 6 is a photograph of the Compex HD heated composite dispenser (AdDent, Inc.) used in this case. Dr. Joshua Friedman of AdDent patented and introduced dental composite heaters (Calset) in 2003. This unique composite delivery gun allows the clinician to place warmed composite directly into the cavity preparation, further enhancing the ability of the composite material to adapt with precision to the cavity preparation. Once the composite is warmed (about 40 seconds), the material is extruded into the cavity preparation between the tooth and the matrix, filling the preparation entirely. Next, using a composite instrument (Mini 4 Goldstein Flexi-Thin, HuFriedyGroup), any excess is removed from the periphery of the matrix, and then the labial portion of the matrix is held firmly against the facial surface of the tooth while the composite is light cured. This will limit the amount of flash, so that there will be very little marginal flash present post cure. Once full cure of the restorative material is completed, contouring the facial “seam” of the restoration to blend with the natural tooth surface, refine facial embrasures, proximal facial line angles (reflective line angles), and incisal edges is accomplished using a series of abrasive discs from course to extra fine (Super-Snap, SHOFU Dental Corporation) (Figure 8 through Figure 10). Next, rubber polishers (A.S.A.P. All Surface Access Polishers, Clinician’s Choice) are used to further polish and enhance the luster of the restorations (Figure 11). A.S.A.P. polishers, by virtue of their unique design, can reach into embrasures and curved surfaces more efficiently than other shapes of polishers to enhance the luster of the composite. Figure 12 and Figure 13 are post-operative views of the completed Class IV mesial composite on tooth No. 7.
Conclusion
Unfortunately, many clinicians place direct composite the same way as they were taught to place amalgam: using pluggers or plastic instruments to “condense” the material into the preparation. Since composite is a pastelike material, it does not behave the same way as amalgam, leaving the potential to create voids between the restorative material and the preparation walls. Add to that the fact that many still layer composites due to the limitations of depth of cure. This also poses the potential for voids between the layers of restorative material. Bulk fill materials help with this but are not considered a cure-all. An advantage of flowable composites is that due to their lower viscosity they adapt well to cavity preparation walls but are difficult to impossible to sculpt or manipulate. However, flowable composites shrink more than conventional composites during polymerization.8 Also, the physical properties of most flowable composites are not sufficient to withstand the forces of occlusion when restoring posterior occlusal surfaces.9 Warming composite gives the benefit of cavity adaptation due to initial lower viscosity, then is sculptable after the heat dissipates. Also, improvements in depth of cure and monomer conversion over traditional placement make warming composite a definite advantage when placing this direct restorative material.
References
1. Woolum JA, Berry TG, Wilson DE, Hatch R, Benefits of preheating resin composite before placement, General Dentistry, vol. 56(4), May 2008, pp. 332-335.
2. Bhagwat S, Mandke L, Vandekar M, Basmatkar N, Pawar A, Khatri R, Longevity of amalgam versus composite resin restorations in permanent posterior teeth: a systematic review, Cureus, 2026 Jul 27;17(7): e88836. doi: 10.7759/cureus.88836. PMID: 40873828; PMCID: PMC12378770.
3. Darabi F, Tayefeh-Davalloo R, Seyedeh-Maryam T, Naser-Alavi F, Boorboo-Shirazi M, The effect of composite resin preheating on marginal adaptation of class II restorations, J Clin Exp Dent, 2020 Jul 1;12 (7): e682-e687. Doi: 10.4317/jced.56625.
4. Abdulmajeed A, et al. Fatiguing and preheating effect on mechanical properties of composite resins, J Dent Res Vol # 98A, Abstract # 1879 (2019).
5. Friedman J, Thermally assisted flow and polymerization of composite resins, Contempory Esthetics and Restorative Practice, Feb 2003, p.46.
6. Wagner WC, Aksu MN, Neme AM, Linger JB, Pink FE, Walker S. Effect of pre-heating resin composite on restoration microleakage. Oper Dent. 2008 Jan-Feb;33(1):72-8. doi: 10.234.
7. Demirel, G., Orhan, A. I., Irmak, Ö., Aydin, F., Buyuksungur, A., Bilecenoğlu, B., & Orhan, K. (2021). Micro-computed tomographic evaluation of the effects of pre-heating and sonic delivery on the internal void formation of bulk-fill composites. Dental Materials Journal, 40(2), 525-531.
8. Baroudi K, Rodrigues JC. Flowable Resin Composites: A Systematic Review and Clinical Considerations. J Clin Diagn Res. 2015 Jun;9(6):ZE18-24. doi: 10.7860/JCDR/2015/12294.6129. Epub 2015 Jun 1. PMID: 26266238; PMCID: PMC4525629.
9. Lopez C, Nizami B, Robles A, Gummadi S, Lawson, N, Percentage and Strength, Modulus, Shrinkage Stress, Translucency, Depth of Cure and Radiopacity, Materials (Basel), 2024 Aug 6;17(16):3901.doi:10.3390/ma1713901. PMID: 39203079;PMCID: PMC11355582.
10. Daronch M, Rueggeberg F, Hall G, Degoes M, effect of composite temperature on in vitro intrapulpal temperature rise, Dental Materials, 23, 2007, pp.1283-1288.